CYTOKINES
 Cytokines have held a special interest for CFS researchers for many years because of their ability, when we have the flu, to produce many of the symptoms found in CFS. Cytokine are not easy to measure, however, and cytokine studies have had decidedly mixed results. Since they play a key role in immune activation, however, groups keep looking. This year was no different from others with researchers coming up with, once again, mixed results.
Cytokines have held a special interest for CFS researchers for many years because of their ability, when we have the flu, to produce many of the symptoms found in CFS. Cytokine are not easy to measure, however, and cytokine studies have had decidedly mixed results. Since they play a key role in immune activation, however, groups keep looking. This year was no different from others with researchers coming up with, once again, mixed results.
A small Lloyd Australian study https://cid.oxfordjournals.org/conten….full.pdf+html underscored the difficulty of getting clear and unambiguous finding from immune studies when the most comprehensive analysis yet of cytokine levels in ME/CFS (35 tests) failed to find any correlation between cytokine levels and CFS. The study was marred, however, by the small number of samples, the high number of tests and the high p value required for significance (p<.005).
Sleep – Many people with ME/CFS feel that if they could just sleep better they could get well. Given the variable evidence for altered daytime cytokine levels, Dr. Natelson wondered if the problem was occurring at night, and got a nice NIH grant to look at that. However, except for increased IL-10 levels (which have shown up several times in other studies) he was unable to find evidence of increased cytokine levels that might help explain the unrefreshing sleep in CFS. He did find some changes but unfortunately nothing dramatic.
We did find some evidence to support a role for an increase in interleukin-10, an anti-inflammatory cytokine. Although the changes were small, they may contribute to the common complaint in CFS patients of disrupted sleep. https://pubmed.ncbi.nlm.nih.gov/20181767
Spotlight on IL-10…The fairly consistent finding of increased IL-10 levels in ME/CFS is interesting – no other cytokine is found to be upregulated as frequently. That finding (thankfully) fits with some other immune findings in ME/CFS. Interleukin-10, for instance, down-regulates several parts of the immune system ( Th1 cytokines, MHC class II antigens) that play a role in pathogen detection. Interestingly for the EBV theory of ME/CFS and questions of autoimmune problems IL-10 also enhances B cell survival, proliferation, and antibody production. It also appears to be an important immunoregulator in the intestinal tract. A study in mice has shown that interleukin-10 is also produced by mast cells. An NIH investigator is looking at whether mast cells play a role in CFS.
Exercise Reveals Cytokine Differences – Underscoring how important stress testing and sub setting may be-while Natelson and Lloyd were finding few cytokine differences at rest, Light found increased levels of a raft of cytokines ( IL-1beta, IL-12, IL-6, IL-8, IL-10, and IL-13 (p<.05) ) in patients experiencing a symptom flare after exercise in this small study (CFS=19). He did not find those increases in patients who did not experience high PEM. Interestingly a recent Pacific Fatigue Lab study also pointed a subset of CFS patients who recovered more rapidly from exercise. Like Natelson and Lloyd (Except for lower CD40L levels) Light found that cytokine levels at rest were similar. https://pubmed.ncbi.nlm.nih.gov/20230500
Cytokine ‘Networks” – Dr. Broderick and Dr.Vernon used data mining procedures to analyze ‘cytokine networks’. Their analyses found the presence of unusual and ‘statistically distinct cytokine communities’ in people with ME/CFS but not in the healthy controls. They suggested that these ‘hub-like’ communities, which they called ‘pre-programmed immune functional components’ might be the result of a “latent viral infection” and they painted a familiar picture of inhibited Th1 immune activation (possibly allowing intercellular pathogens to flourish (remember IL-10)) and increased Th2 activation (possibly resulting in increased allergy and auto-immune problems) and impaired NK cell responsiveness.
Cytokine studies in ME/CFS have had mixed results but here they noted that simply measuring cytokine levels was insufficient for understand immune functioning in CFS – which, if you think about it, is probably true in any disease. The immune system, after all, is unbelievably complex and simply charting the highs and lows of any part of it, can hardly describe the interactions taking place within it. The network analyses these researchers did were an attempt to get a systemic look at a live and complex community. Their findings that a ‘latent viral infection’ might be present fit the latent herpesvirus theories of Lerner, Glazer and Montoya. Finally they posited areas of the immune system that might be targeted for treatment.
These observations are consistent with several processes active in latent viral infection and would not have been uncovered by assessing marker expression alone. Furthermore this analysis identifies key sub-networks such as IL-2:IFN-?:TNF-? that might be targeted in restoring normal immune function. https://pubmed.ncbi.nlm.nih.gov/20447453
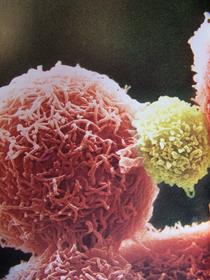 Natural Killer Cells and Chronic fatigue syndrome
Natural Killer Cells and Chronic fatigue syndrome
Natural killer (NK) cells are a different ballgame; NK studies do tend to have consistent results and this years studies were no exception. (The photo on the right is of a NK cell in yellow taking on a red tumor cell)
NK cell findings validated – A VERY small Brenu Australian study (n=10) validated several important immune findings in ME/CFS while failing to validate red blood cell abnormalities. It confirmed significant decreases in CD56brightCD16- NK cells levels, confirmed that decreased NK cytotoxic activity was present and demonstrated for the first time significant reductions in neutrophil respiratory burst – a finding that nicely correlated with an earlier MERUK study which found increased neutrophil apoptosis or death. (When immune cells get triggered by a pathogen they often undergo a ‘respiratory burst’ as they turn on their defenses and ramp themselves up into pathogen killing machines.)
This small study suggested that neutrophils in CFS patient may have trouble getting themselves into ‘fighting shape’ and in doing so perhaps displayed yet another instance of ‘stress induced failure’ in ME/CFS. The authors noted that similar findings are found in rheumatoid arthritis and other immune diseases. This group could clearly use more funding.
Reduced NK CD56brightCD16 – NK cells have also been observed in patients with coronary heart disease, allergic rhinitis and juvenile rheumatoid arthritis, in all cases NK cytotoxic activity was also reduced. The reduction in cytotoxic activity was explained by a reduction in IFN-? producing CD56brightCD16- NK cells which led to poor cytotoxic activation. https://pubmed.ncbi.nlm.nih.gov/20077123
Natural Killer Cells AND a Biomarker? – In this paper the authors noted how complex CFS is and the difficulty there has been in finding consensus on immune issues but then noted the one area that consensus has been achieved – natural killer cells dysfunction.
Like many chronic illnesses CFS pathophysiology is complex….although reviews of the immunology of CFS noted that universal agreement of immunological abnormalities had not been achieved, in no small part due to differences in methodologies,case definition and study quality.
Study quality is always a big issue with CFS studies because many of them are done on a shoestring which can impact study design and scope. Neither of those are issues with NIH funded studies which tend to be quite large and quite rigorous. Dr. Fletcher and Dr. Klimas have really been quite adept (relative to other researchers) at getting NIH grants and this was one of them. (In fact the funds for this study came from no less five NIH grants and four Institutes and the CFIDS Association of America – suggesting that getting the funding may have been the most complicated part of the study )
This large study found that NK cell killing ability was significantly reduced in people with ME/CFS (n=176!) vs healthy controls (n=230). It also found that people with reduced natural killer cell functioning tended to be sicker as well. Showing that a finding is associated with ‘illness state’; ie symptoms is very important for convincing the research community that it actually plays a role in the illness.
Interestingly this is yet another study which showed that the way to get at ME/CFS is not to look at the system in stasis (NK cell numbers were normal) but to look at it in action which in this case meant analyzing how effect the natural killer cells were at doing something (killing pathogens). is nothing like a large study to really cement findings in the research community and this study should do that in spades with regards to the natural killer cells in this disorder.
The other major finding were the reduced levels of the CD26 marker on lymphocytes and reduced enzyme levels in the blood. This protein is an immune and metabolic regulator and low levels could suggest the inability of immune cells to become activated or for low-grade levels of inflammation to be present (ie metabolic syndrome). Although it has not been particularly well studied it also appears to play a role in tumor suppression.
As with the cytokine network study the results were also suggestive of increased Th2 activation in ME/CFS and which could result in the reduced ability to attack intracellular pathogens such as viruses and possibly have autoimmune manifestations as well. The group also linked the abnormalities to T-cells, which would, with the attention given to those heavy hitters of the immune system, would be a huge win for ME/CFS. All in all this is a very strong paper for ME/CFS.
The decreased NKCC and the abnormal DPPIV/C26 manifestations in CFS would be compatible with the hypothesis that the immune system of affected individuals is biased towards a T- helper (Th) 2 type, or humoral immunity-oriented cytokine pattern. The data obtained on NK cell function, immune activation and DPPIV/C26 on cell surfaces and in serum, are consistent with a viral etiology for CFS. The elevated proportion of activated CD4 and CD8 T cells and defective NKCC in CFS cases suggests that T cells are metabolically limited in performing their helper function. The abnormalities observed may have applications with other complex, chronic and poorly understood illnesses, including fibromyalgia, gulf war illness, rheumatologic disorders and multiple sclerosis—though the precise constellation of patterns observed with these biomarkers may differ in each. However, the specific panel that we have identified here are likely to be helpful as objective markers for diagnosing CFS, determining subgroups, following patients over time and as targets for therapeutic strategies. https://www.ncbi.nlm.nih.gov/pmc/arti…7/?tool=pubmed
 PATHOGENS
PATHOGENS
Enteroviruses in chronic fatigue syndromeParvovirus Infection – Drawing a remarkably similar conclusion to Lerner but with regards to parvoviruses, not herpesviruses, Kerr found evidence of a ‘hidden’ B-19 infection. Kerr found no evidence of increased parvovirus infection when looking for antibodies to its structural (later proteins) but ample evidence of parvovirus infection (42%) using non-structural proteins.
This appears to suggest that a kind of smoldering infection that pumps out gene products (non-structural proteins) but not actually viruses (structural proteins) may be present in ME/CFS. If I’m reading this right this could suggest that some people with ME/CFS have trouble completely controlling the virus in a similar manner proposed by Lerner with EBV.
The antibodies he found in ME/CFS are thought to indicate chronic or severe courses of B19 infection. Kerr has been well-known for his willingness to collaborate and this study included a bevy of well known ME/CFS researchers and physicians including Dr. Chia, Dr. Komaroff and Dr. Enlander.
As NS1 antibodies are thought to indicate chronic or severe courses of B19 infection, these findings suggest that although the seroprevalence of B19 in CFS patients is similar to controls, the immune control of the virus in these patients may not be efficient. https://pubmed.ncbi.nlm.nih.gov/20007355
Herpesviruses Not Found – Lloyd has made the immune and pathogen rounds in his Dubbo participants – each of which had infection triggered ME/CFS. He has looked for bugs and immune factors and except for high cytokine levels at the very start of the process he has, to his own surprise, struck out. Here he uses PCR and looks for antibodies to herpesviruses (EBV, HHV6, CMV) and finds no evidence of herpesvirus reactivation in people who ended up coming down with ME/CFS compared to those who recovered. The caveat? – this was a VERY small study – consisting of only five patients and controls.
These data do not support the hypothesis of ongoing or reactivated EBV, HHV-6, or CMV infection in the pathogenesis of CFS. https://pubmed.ncbi.nlm.nih.gov/20827765
Herpesviruses Found – Kerr, however, found plenty of evidence of herpesvirus reactivation in his interesting (and much larger (n= 111 CFS patients)) gene expression and pathogen study in people with ME/CFS and healthy controls. Herpervirus ‘seroprevalence’ or the percentage of people infected with these common viruses was equal in the two groups but when they looked at evidence of reactivation (using EBV markers VCA IgM, VCA IgG, early antigen IgG and EBNA IgG) they found a whopping increase in EBV reactivation in ME/CFS with (p<0.007) with 100/111 patients having reactivated EBV infections vs only 28 controls.
They were also able to establish that 61 people were in the primary/reactivation phase and 39 in the late phase. The fact that twelve of the 88 genes that are abnormally expressed in the CFS group were associated with EBV provided indirect validation of their findings.
They also found evidence of parovirus and enterovirus infection in 12 and 6 patients respectively. This was a strong study that validated past herpesvirus study results and provided additional evidence that they were present.
Antibody testing for Epstein Barr virus, enterovirus, Coxiella burnetii and parvovirus B19 revealed evidence of subtype-speci?c relationships for Epstein Barr virus and enterovirus, the two most common infectious triggers of CFS/ME. https://www.ncbi.nlm.nih.gov/pmc/arti…/jcp072561.pdf
Takeaway Points
All in all a good year for immune research. There were not a lot of studies but those that took place tended to be successful and should push the field forward.
- Cytokines – the cytokine picture in ME/CFS remains muddy although the Light study suggested that submaximal exercise and subsetting according to symptom presentation might be what’s needed to propel this field forward.
- Natural Killer Cells – the most consistent immune finding was validated in a big and linked to symptom presentation plus low levels of an enzyme could help explain why NK cell activation is so poor and could end up being a biomarker for this illness.
- Pathogens – the natural killer cell studies which suggested an infection could be driving ME/CFS were backed up by two studies demonstrating that herpesvirus, parvovirus and enterovirus infections are increased in people with ME/CFS.
- Whither Kerr? – Kerr has co-authored several important pathogen and gene expression studies. His latest gene expression study accomplished what no other gene expression studies in ME/CFS have been able to achieve – replication of their prior results. Kerr’s gene expression study also provided indirect evidence of EBV infection in ME/CFS. Kerr’s bid for tenure, however, reportedly failed which could affect his ability to continue with ME/CFS research. Will he be able to remain active in ME/CFS research?
